Types of Pregnancy Loss
[A note about medical terms: In medical language, “abortion” means the ending of a pregnancy by death and does not indicate the means. This is a hard word to read or hear because if you have suffered the loss of your child, the last thing you want to feel is that someone is accusing you of aborting him. Throughout the site I am not using the technical word abortion, but I am inserting the medical terms below so that if you come across them you will understand what they mean. “Abortion” was hard for me to hear too, and I was used to it.]
Chemical Pregnancy or Early Pregnancy Loss: a miscarriage that occurs before six weeks.
Blighted Ovum or Empty Sac: The gestational sac develops and is able to be seen on ultrasound, but there is no sign of a baby inside the sac. This will only occur very early in pregnancy. Many times women are scheduled for additional ultrasounds because it is possible that the pregnancy is not as far along as thought and thus the baby is not yet visible on ultrasound.
Spontaneous Miscarriage (Spontaneous Abortion): A miscarriage that happens on its own, without medical intervention. This may result in a Complete Miscarriage (Complete Abortion) or an Incomplete Miscarriage (Incomplete Abortion). In the former, everything in the uterus is expelled, including placenta. In the latter the uterus is not fully emptied and usually medical intervention is necessary. Some data suggests that in pregnancies over 12 weeks the placenta is more likely to be retained. It is necessary to completely empty the uterus to avoid hemorrhage and infection. An incomplete miscarriage that results in infection is called a Septic Abortion. There is a risk that this can progress to a life-threatening condition called septicemia (“all over” infection).
Missed Miscarriage (Missed Abortion): The baby has died (or only a sac is seen) but the actual miscarriage has not yet begun. Many miscarriages are actually “missed” at some point, but the miscarriage process begins before this is detected. Waiting for miscarriage to begin on its own is considered a natural miscarriage (to be discussed more below).
Threatened Miscarriage: There are signs that a miscarriage may be in progress or may take place, but it is not certain. Some pregnancies progress normally after this diagnosis and some end in miscarriage. Sometimes (depending on gestation) women are put on bed rest at this point.
Ectopic Pregnancy (Tubal Pregnancy): The baby has implanted outside of the uterus, usually in one of the fallopian tubes. The fallopian tube is very small and not capable of distention past about 8 weeks (there are always exceptions) with most ectopic pregnancies being detected by 6 weeks. Ectopic pregnancies are considered completely non-viable pregnancies, the continuing of which will endanger the life of the mother. If the tube ruptures, apart from severe pain, the woman may have heavy bleeding to the point of going into shock. This also eliminates one tube which will lessen her chances of conceiving in the future. Depending on the size of the baby, medication (methotrexate) may be given to end the pregnancy (the woman will experience bleeding similar to a regular early miscarriage) or, if too large, surgery may be done to remove the tube and baby. Time is considered of the essence in this situation. (More information on ectopic pregnancies can be found in the medical and surgical sections below.)
Stillbirth: The delivery of an infant who died either in utero or during the process of birth. In Australia this is defined as 20 weeks gestation and beyond. In the UK, this is defined as 24 weeks and beyond. WHO defines this as 24 weeks and beyond. In the US, there doesn’t seem to be an “official” definition, but it is commonly assumed to be 20 weeks and beyond.
Management of Pregnancy Loss
Medical:
1. Intrauterine pregnancy (missed abortion)
When you choose medical management, your doctor or midwife will give you medications to help your uterus contract and expel its contents. The most commonly used medication is misoprostol, which causes intense cramping of your uterus. Your doctor or midwife will also usually give you a medication for pain. Misoprostol often causes diarrhea and may cause some nausea. Let your doctor or midwife know if you aren’t able to keep the medicine down. You will usually have to take two doses of medication about 6 hours apart. Medical management of miscarriage is generally effective within 24-48 hours. You can expect less bleeding than with a natural miscarriage, but should still be prepared.
Misoprostol can also be given vaginally and less commonly, rectally. If using vaginally insert the pills as far up in the vagina as possible and lie down immediately afterward. It is a good idea to plan to do this at bedtime. You may also want to take pain medication at the same time. Try to stay horizontal so the pills stay in the right place so they can work. This dose may also have to be repeated. Some women notice less nausea and vomiting with the vaginal method.
If you are past the first trimester, expect to be admitted into the hospital for administration of the misoprostol. Otherwise, you will safely be able to do this at home. The management for the miscarriage once it starts is the same as found below in the Expectant Management section. [Note: my second loss (13 weeks) was managed by induction of labor by misoprostol in the hospital. The story is found on the “Your Stories” page at the very bottom, “Andrew”.]
2. Ectopic pregnancy
Your doctor or midwife will probably offer you several different ways to manage your miscarriage. As mentioned above, the medical term for a miscarriage is abortion. It is important to understand that there is not necessarily a right way to manage a pregnancy loss. It is also important for you to understand that your doctor or midwife may be advising you based on her personal experience and preference.
An ectopic pregnancy is a pregnancy that is “out of place” (the literal meaning of the term). Most non-medical people refer to this as a “tubal pregnancy.” Ectopic pregnancies most commonly occur in the fallopian tubes, but they may also occur in the cervix, the cornua (area of the uterus where the tube enters), ovary, or the abdomen. Ectopic pregnancies are serious and are a significant cause of maternal death in the first trimester.
I think there is sometimes a misconception that an ectopic pregnancy is somehow different in terms of what the baby looks like. All things being equal an ectopic pregnancy is the same as an intrauterine pregnancy…just in the wrong place. Below is a photo of a baby in the sac removed at 6 weeks because of implantation in one of the fallopian tubes. The baby was still moving until the sac was opened.
 |
| [I believe this may be in fact 6 weeks after conception, not 6 weeks post LMP, making this really an 8 week baby.] |
Your doctor or midwife may suspect an ectopic pregnancy because of your symptoms or because she doesn’t see anything in your uterus on an ultrasound. If your pregnancy hormone (beta HCG) level is above 1500, it should be possible to see a pregnancy in the uterus. Your doctor may also order a progesterone level to help evaluate the pregnancy. A progesterone level of less than 5 indicates an abnormal pregnancy; a level greater than 25 indicates a normal pregnancy. Most women, however, have levels between 5 and 25. Your doctor or midwife may have you return in 48 hours for a repeat check of your pregnancy hormone level. In a normal pregnancy, the level should increase by two thirds in 48 hours. A hormone level that does not go up as much indicates an abnormal pregnancy. If no sac was seen in the uterus, this implies an ectopic pregnancy.
Expectant management of an ectopic pregnancy is similar to that of a missed abortion or blighted ovum. Your doctor or midwife may have you return in 48 hours for a repeat check of your pregnancy hormone level or may have you wait until the next week. You will be given strict instructions on symptoms that should lead you to call your doctor. DO NOT IGNORE THESE SYMPTOMS. A ruptured ectopic pregnancy is a true medical emergency. If your hormone levels are decreasing and you are not having symptoms, your health care provider will continue weekly checks of your pregnancy hormone level until it reaches zero.
Some women opt for medical treatment of an ectopic pregnancy. If you choose medical treatment, you will be given a shot of methotrexate. Methotrexate is a drug that prevents genes from being copied and prevents proteins from being made. It causes the placental tissues to die. Before you get methotrexate, your doctor will check to make sure that your liver and kidneys are functioning properly. Methotrexate is given as an injection into the muscle (usually the buttocks). You will have your pregnancy hormone level checked on the day you get the shot, the third day after the shot, and the sixth day after the shot. It is normal for the level to go up between days 1 and 4. Your doctor or midwife will look for the level to drop by 15% between days 4 and 7. If the hormone level does not drop enough, you and your midwife will need to discuss whether you should get another shot or whether you should have surgery. If it does drop enough, you will continue to have your pregnancy hormone level checked each week until it is negative.
Methotrexate has many side effects, including diarrhea, nausea and vomiting, and abdominal pain. There are some rare cases in which methotrexate causes the bone marrow to temporarily stop making blood cells. This only lasts for a short time and is reversible.
Surgical:
1. Intrauterine pregnancies: Dilation and Curettage (D&C)
There are numerous places online that detail exactly what happens during a D&C. A good example in layman’s terms can be found
here or
here. Technically, few D&Cs (which involve scraping the uterus with a sharp instrument) are performed any more. The usual procedure for emptying a uterus because of miscarriage is called
vacuum extraction or a suction D&C. D&C has come to be the generic name for all such procedures. There are also cases in which a combination of suction and curettage is used. In a nutshell, this is what to expect:
The day before the scheduled surgery you will go to the hospital for preoperative lab work and to be evaluated for anesthesia. This will probably take a few hours. You will be instructed not to have anything to eat or drink after midnight. If you are on medications, you will be discussing which ones to take and which ones to hold.
A D&C is an outpatient procedure so unless there are complications you will not be staying overnight. You will register in the preoperative department and spend some time there getting an IV placed, receiving any sedation, etc. The nurses will make sure that everything is in order, all consents are signed, and you have questions answered. Then you will be taken into the OR. Usually there are two options for anesthesia: conscious sedation and complete sedation. In the former, you are awake, but not very aware, and you shouldn’t feel any pain. You may feel some pulling sensations during the actual procedure. In the latter you are put to sleep and you wake up in the postoperative department. The anesthesiologist will have discussed these options with you and it will be your choice.
You will be positioned in the lithotomy position on the operating table (just like a regular gyn exam). Your legs will be securely propped up so you do not have to hold them there. You will be given oxygen and your vital signs will be monitored. You will have electrodes attached to your chest and arms (this doesn’t hurt) to monitor your heart. At this point you should be drifting off.
The doctor will use a speculum to open the vagina. It will stay in place the whole time. Dilators of increasing size are inserted into the cervix to widen the opening. When it is open enough a tube is passed through it into the uterus. Suction is applied through the tube to remove everything in the uterus. [Note that this is a blind procedure and the doctor stops when he ‘thinks’ he has removed everything. Sometimes this was not the case and a repeat D&C must be done.] When the doctor feels the uterus is firm enough (it will cramp very hard during the procedure) and the bleeding is within reasonable limits you will be taken to the postoperative department to recover. Everything that was removed from the uterus is collected, examined for completeness, and sent to the pathology department. The entire procedure takes only about fifteen minutes.
You will stay in recovery until you are awake, your vital signs are stable and close to the levels they were when you were admitted, you can tolerate fluids by mouth and you can urinate. Your bleeding will be monitored and if it is found to be too heavy, you may stay longer or possibly be admitted. You will be given medication for pain. You will not be able to drive yourself home so make sure you brought someone with you. You will be given detailed instructions for how to take care of yourself at home.
Bleeding may last up to two weeks (similar to that of an unassisted miscarriage) but will probably be less than a regular period since most of the superficial lining of the uterus was removed during the procedure. The rest of your care is identical to that after an unassisted miscarriage (see that section). You may be given antibiotics to take to prevent infection.
Complications are rare (less than 1 in 100) but include infection, excessive blood loss, perforation of the uterus and uterine adhesions (which may affect the ability to be pregnant again). I strongly recommend going to
this site to read more about the risks of D&C. Here is the statement on the home page of DandCnow.info:
There are many websites that include descriptions of the surgery, D&C, in detail and what to expect before, during and after the surgery. However, apparently there are no websites specifically devoted to providing education about this surgery based upon current medical research. In addition, this website offers a more comprehensive picture of a D&C by educating from several perspectives: medical research, experienced gynecologists’ perspectives and women’s experiences. All of these facets provide the reader with a more comprehensive view of the surgical procedure, known as dilation and curettage. It is our hope that through this website, a dialogue will begin, which will reassess the merits of D&C and the value of emerging and established alternative treatments. Hopefully this dialogue will lead to the greater use of less invasive gynecological practices.
2. Ectopic pregnancies: Laparoscopy
Some women choose to have surgery to remove an ectopic pregnancy so that the process will end more quickly. In other cases, the doctor will recommend surgery because of the size of the ectopic pregnancy or because she suspects that you are bleeding. If your doctor believes that you have a ruptured ectopic pregnancy, you need to have surgery. Ruptured ectopics are medical emergencies and are fatal if not treated. While no one can make you have surgery if you refuse, you should know that a doctor who uses the term “ruptured ectopic” believes that surgery is necessary to save you.
Surgery is usually with a camera that allows the surgeon to operate without making a large incision on your abdomen. This is called a laparoscopy. Laparoscopies are generally outpatient procedures. Your pre-operative experience is the same as that described above in the section about D&C.
In the operating room, you will be put to sleep. A small incision will be made in your belly button and a camera will be inserted. The surgeon will look around with the camera and then make two other small incisions in line with your hipbones and below your belly button. She will clean out the blood in your belly and then decide how to best remove the ectopic pregnancy. If the ectopic is small and the tube looks relative normal, she will make a small slit in the tube and gently extract the ectopic (a salpingostomy). If the pregnancy is large or the tube looks very abnormal, then she will likely remove the entire tube (a salpingectomy). You can still get pregnant with a single fallopian tube. Your postoperative experience is similar to that described above in the section about D&C.
Less commonly, you will have to have surgery through an large incision without a camera. This is called a laparotomy. You may have to have this type of surgery if you have too much bleeding to have surgery with the camera, if you have had abdominal surgery before, or if you have an ectopic that is outside of the fallopian tube. The surgeon will usually make a “bikini” incision and then examine your tubes and ovaries. You may have a slit made in the fallopian tube or the entire tube may need to be removed. After a laparotomy, you will be admitted to the hospital. You will usually stay for two or three days after surgery.
If you have had significant bleeding, you may need a blood transfusion. If your blood type is Rh negative, you should be given Rhogam.
Expectant Management:
This is also known as the “watch and wait” choice and in this blog is usually referred to as “natural miscarriage”. You may wait a few days or you may wait a few weeks from the time you learn your baby has died. Most women will deliver within two weeks. Also, once the active miscarriage starts, it may start slowly and progress over a few days or it may be over in a matter of a few hours. The length of time does not correspond to the length of the pregnancy. At 12 to 13 weeks my “active” miscarriage took 3 1/2 hours from spotting to delivery of the last clot.
Especially in the first trimester this is a reasonable option for most women. While you are waiting you may be asked to go into your doctor or midwife’s office for vital sign checks and/or labwork. If you start to feel ill during this time you need to call your practitioner immediately. (See “When to seek medical attention” below) If after several weeks you have still not delivered you will need to talk to your practitioner and review your options because your risks of infection and blood clots have increased.
[Below this section there is a discussion of the pros and cons of each method and the factors that play into choosing each. While you should always discuss this with your doctor, you should also be informed of your options and this does not always happen in the doctor’s office. In the end, the decision will be up to you.]
Preparing:
It’s always good to be prepared. It gives you something to do and you will feel more in control of the situation. You will need:
-
very large sanitary pads and a decent number of them
-
a container to put the baby in
-
absorbent under pads (chux)
-
at least one old towel
-
scissors (just in case)
-
something to drink
-
cold washcloth (for you)
-
(optional) strainer to use while on the toilet
I recommend the chux because 1) there will be a lot of blood – (it’s easier to use the chux (they have a water-proof backing) and throw them away) and 2) there will be a good number of sizable blood clots and the placenta and the chux are convenient for disposing of them neatly.
*Note: Although it is perfectly possible to undergo a natural miscarriage on your own, if you are more than a few weeks along it is advisable to have someone else in the house with you, if not in the same room. At best you will have moral support and at least you will have someone to call on in an emergency. If it is unavoidable that you are alone, have a phone within reach in case of emergency.
Signs of impending miscarriage:
-
cramping, period cramps or harder, sometimes approximating labor pains
-
spotting – will probably start brownish and then turn red
-
sometimes an upset stomach
Sometimes you will simply be surprised. If this happens it is at least likely to be quick. If you notice any signs of spotting or just ‘have a feeling’ it’s coming, go ahead and assemble your supplies and if you are alone, call someone to be with you. I advise putting a pad on and/or a chux under you. When the bleeding starts in earnest, it is very likely to be sudden and dramatic.
Managing the actual miscarriage:
If you have been waiting for a while to miscarry, as in the case of a missed miscarriage, then you may be relieved to have the process finally starting. You may also be overwhelmed with grief or panic. Keep in mind that women have been miscarrying at home for thousands of years. This is where having a support person can be very helpful. Take a deep breath and say a prayer. If it helps, place an icon where you can see it.
On dry land:
If you are most comfortable on your bed or the floor (I don’t recommend the couch), then you will be very, very glad that you have chux available. It is a good idea to put down a layer of four or more chux so that one can be removed easily and another one waiting. There is no scripted position. Sit, crouch, kneel, whatever. The position that makes you the most comfortable is likely to change throughout. Do whatever feels better. Do be in a position that you have something to lean back against if you need to. This can be another person. You may feel faint at some point and need the support.
In water:
Most women find warm water eases the pain associated with cramps and the water helps support your weight so positions are easier to hold. The water may be psychologically helpful because after a very few minutes the water is mostly opaque and you cannot immediately see anything you’re not ready to see. The bathtub also provides a natural backrest and handholds. Changing positions when in the tub is the same as on dry land. When you are done delivering everything you can clean up right in the tub instead of transferring. Place a few chux on the floor next to the tub so you can keep everything tidy when you get out (and to provide a place to put things if necessary).
On the toilet:
Some women find this position to be most comfortable. I recommend having a strainer in place so you don’t have to retrieve the baby from the toilet – this can be emotionally painful. The advantage is that you can flush the clots rather than having to dispose of them otherwise. I do not recommend flushing the placenta unless it is fairly small. At between 12 and 13 weeks of growth my placenta was easily 9 inches across and thick. If you start to feel faint while on the toilet, then quickly move to the bathroom floor. Better that than to fall. Place a chux or two on the floor under your feet.
(From here on out everything is the same regardless of your chosen position.)
My miscarriage began with a sudden rush of blood (after initial cramping and spotting for a few hours). Very soon after that I delivered the amniotic sac (containing the baby) and a large clot. You may pass several clots first.
After delivering the baby feel free to “stop” and hold him. If he is in the sac, carefully open it up.** Having wet hands helps hold the baby because of his fragile skin. Take some time to hold him and talk to him. You are not in any hurry here. When you are ready, place him in the container (I suggest having water or saline in it) so you can finish passing everything. One reader asked that I note that if you want to rinse something off, it is better to “swish” the sac/baby/placenta/tissue in a container of water rather than run the tap over it due to the delicacy of what you’re handling. You can also take advantage of the container of water/saline to hold the baby in your hand while it is submerged in the water. At least one example of this is on the photographs page.
It may happen that when you deliver the sac you notice the cord is still attached. Don’t pull on it; go ahead and cut it (there’s no need to tie it off).
 |
| Gabriel (my third miscarried baby) still in the sac. (11 weeks) |
 |
| Thea’s 6 week twins in separate gestational sacs. |
** Depending on how long it has been since the baby died, you may see something different in terms of the sac. Usually the amount of amniotic fluid decreases over time so depending on how much there was to start with, you may or may not see a nice, full “bubble”. In addition (and this is important), the uterus will form a clot around the sac/baby as time goes on. This means that you may deliver the baby in the sac very obviously, or you may deliver a sac with a clot attached, or you may deliver what appears to be a large clot or placenta but which is actually the sac enclosed in a clot. Especially if you feel as though you are completing the miscarriage but haven’t seen the sac, check inside the large clots. This sounds gross, but it will feel a little different when you are looking for your baby. The clot will be on the sac, not the baby (all things being equal) so you will still be able to remove the baby from the sac if you so desire. When my first son was born his sac had a large clot attached. It covered about 1/3 of the surface. When my second son was born there was no clot attached at all.
For example, here are some photographs of Thea’s twins. Their amniotic sacs and placenta were surrounded by clot which had to be manipulated before the babies came into view.
Thea: “This is what the tissue looked like right after I miscarried:”
“Moving away blood and clots uncovered the gestational sac with placenta attached and some weird tubular-shaped membranous tissue off to the right. I could see two tiny white bodies through the gestational sac.”
“After ripping open the gestational sac the two amniotic sacs came into better view. The sacs were very close together before I spread them apart to take the photo. The tiny babies are inside the sacs, one just above the 10 and 1/4 inch mark and the other just above the 11 inch mark.”
[You can see the rest of the pictures of Thea’s twins on the Photographs page.]
For another example, when Kristen delivered her son, Ryan, at 13 weeks, he was encased in this mass of tissue:
Between the time you deliver the baby and the placenta you are likely to pass several clots and a lot of blood. A word about the blood: Just as you don’t panic when you have a very heavy period, do not panic now. This blood is mostly endometrial lining sloughing off and not directly out of your blood vessels. As the placenta detaches you will have some “active” bleeding, but we’ll talk about that in a moment. The clots are not tissue, they are just that – clots. Whenever blood sits for any time it clots. This is what it is doing inside you. Some will be large, the size of your palm. The blood will be a steady trickle with occasional gushes (as a clot is moved out of the way). If there is a problem later and you need to tell someone how much blood you passed, you will be able to mention the number of chux used. (Yes, this is the one disadvantage of an in-water miscarriage.)
The placenta may come out rather quickly or not. You do not want this to take a long time – say, not much more than an hour. The uterus will not stop bleeding until it is able to tightly clamp down (remember, it’s like a big muscle) and it cannot do that if anything is still inside. Thus, you will continue to bleed and pass clots until the placenta is delivered. If it feels like it’s been a while, you can do something very simple to encourage it to come out. (And, by the way, do not pull on the cord. It won’t work at best and at worst you can cause damage.) You have probably already been able to feel your fundus, the top of the uterus. Find it now and massage it very firmly. Don’t punch yourself, but rub slowly and deeply until you feel strong cramps beginning. Continue to massage for another minute or so to make sure the cramps will continue. The cramps are the uterus contracting to try to expel the placenta. Go by how you feel here, but after a few minutes try bearing down. Do this a few times. If the cramping subsides, massage your fundus some more. This is almost certain to result in the delivery of the placenta in under ten minutes. If more than an hour has gone by, you are still bleeding copiously, and there is no sign of the placenta, consider getting medical assistance. Sometimes placentas are embedded very deeply in the uterine wall and are difficult to expel. We will talk more about when to call for help below.
When the placenta is delivered if it is intact you will (hopefully) find it unmistakable. [Reference photos below.] The maternal side (the side that was against the uterine wall) will look like raw hamburger – sorry. The baby’s side will be covered with a shiny “skin” and will look more purplish. Blood vessels will be seen leading toward the umbilical cord in the center. Put the placenta on a chux and have a good look at it. It should be round to ovalish in shape and will vary in size with the length of the pregnancy. There should not appear to be pieces missing from the edge (which would lead one to believe part of the placenta is still in place). If you are not sure what you are looking at, or if the placenta is complete or not, don’t hesitate to put the placenta in a watertight container to take to the doctor. If the placenta does not appear to be complete and if you have not delivered all the pieces, then you will need to seek medical attention. A D&C may have to be done to remove the remaining part(s). Alternately, your placenta may deliver completely but in pieces. You can tell the placenta from the clots because the clots are easily broken up. The placenta will feel more “fibrous”.
 |
| Full-Term: Maternal side (source) |
 |
| Full-Term: Fetal side (source) |
Placenta size can vary significantly depending on the length of the pregnancy. In a missed miscarriage the placenta may keep growing for several weeks until the body recognizes that the baby has died. The placenta below is from a baby measuring 6 weeks, 1 day, but not miscarried until 14.5 weeks. (There are more photos on the Photographs page: Selah Lael 6 weeks, 1 day.)
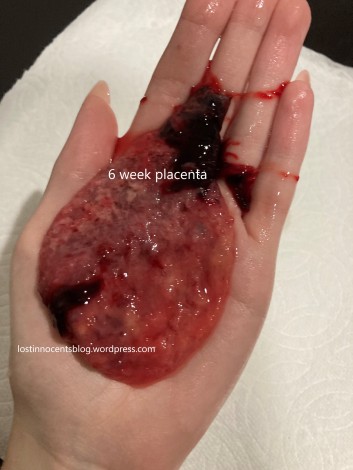
Below is a photograph of a placenta with (collapsed) sac attached (and possibly some clot attached too) generously donated by Allison. Her baby died at 7 weeks and she miscarried at 11 weeks. The doctor confirmed that this is what she was looking at.
 |
| 7-11 Week Placenta |
Below are two photographs of a placenta from a twin pregnancy. In the first you can see 11 week Arrow on top of the placenta. In the second you can see a gestational sac containing 5 week Cedar on the bottom edge of the placenta. The entire placenta is a little larger than my palm (per other photos with scale context). (You can see additional photos of Cedar and Arrow on the Photographs page.)
Heavenly miscarried again later this year and sent photographs of her baby (Zion) and placenta, shown below.
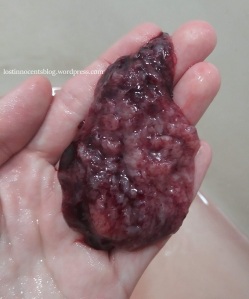
Placenta delivered with 9 week pregnancy

Placenta (left) and probable partial placenta (right) delivered with 9 week pregnancy
Below are two photographs of the placenta I delivered with my third baby, Gabriel. He died at about 11 weeks and was delivered 19 days later. While the placenta was delivered all at once, it was not intact. It appeared to have torn 80% down the middle. If put back together it would be approximately the area of my hand (5 in x 6 in). (I’m sorry the first photo is a bit blurry. I was pretty faint from blood loss at this point and can’t believe I managed to take pictures at ALL.)
 |
| 11- 13 week placenta: Maternal Side |
 |
| 11- 13 week placenta: Fetal Side |
This photograph was just submitted by a woman who delivered her 11 week, 5 day baby in the hospital at 14 weeks, 1 day. You can see the difference between the placenta on the right and the blood clot on the left.
 |
| 12 week placenta on right, blood clot on left. |

placenta from 13 weeks, 6 days pregnancy
 |
| 7-8 week placenta (top) and umbilical cord |
[There are some additional photographs of babies in sacs with or without placentas on the Photographs page.]
After the placenta is delivered you will still pass some more blood, probably a gush behind the placenta, and possibly some more clots. This should decrease quickly after the placenta is out however. The cramping and pain should decrease significantly at this point too. If you are taking something over the counter for pain, take acetaminophen rather than ibuprofen because the latter can increase bleeding.
Afterward:
When you are ready, clean up using cool (not cold, unless you want to) water. Warm to hot water will make the blood harder to remove. Put on a pad and lie down. If you have not been sipping all along, drink a full glass of something at this point. You will have lost fluid volume and need to replace it. Do not take this opportunity to clean the entire bathroom. If you do, you will wind up passing out or very nearly (like I did).
At some point I recommend you take photographs of the baby. If you simply can’t do this, have someone else do it. Even if you don’t want to see the pictures now, you will probably want to see them later and it will be nice to have them. Take lots. Take photographs of details. Put wedding rings or something next to the baby for scale. You need never share these photos, but you may wind up treasuring them yourself. After taking photographs, place the container containing the baby in the refrigerator. This slows decomposition.
[Note: After my third loss I was really faint from loss of blood and very exhausted. I left Gabriel in the sac in the container of water. I took a few pictures, but waited until the next afternoon when I was physically more recovered and more emotionally ready to proceed. Don’t feel like you have to rush.]
Recovery:
After you miscarry call your doctor. They will almost certainly want to see you for a follow-up ultrasound (to see if the uterus is empty) and an exam. Expect to bleed for about one to two weeks. The pattern may be stop and start. Eventually the discharge will change from red to brown to tan. If the bright red bleeding persists after this, check with your doctor. There may have been something retained in the uterus that was not previously detected. Use pads, don’t use tampons. Do not insert anything into the vagina until you have stopped bleeding. Do not do any heavy labor, strenuous exercise, etc., during the first several days at least. Get extra rest. Make sure you drink enough fluids. Take a few days off from work. Even if you have a desk job, you will probably not feel up to facing anyone yet.
One thing that people are not told to expect is some depression. Obviously, there is the grief from losing your baby, but there are other factors at play. When you deliver, whether at 8 weeks or 40, the hormones that have been very high during pregnancy drop precipitously. This is usually referred to as “the baby blues” and if more severe or persistent, “postpartum depression”. What most people are not aware of is that women who miscarry are at as least as much risk for postpartum depression as women who deliver live babies and usually more. If you have delivered a living baby you will be distracted by the care of a newborn and you will be surrounded by balloons and flowers and congratulations. After a miscarriage you not only do not have these, but you have the added grief of pregnancy loss. There is an excellent article on depression after miscarriage here. Do not hesitate to get help if this is becoming a problem. Pills will not make grief go away, but you may need some support for the physical causes of depression.
When to seek medical attention:
-
Fever over 100 degrees F
-
Severe abdominal pain or pain that is increasing (except the normal increasing of cramps until the baby is delivered)
-
Nausea and vomiting (some women experience this during the actual miscarriage – that’s ok)
-
Difficulty urinating
-
Foul-smelling vaginal discharge
-
Bleeding that saturates a pad an hour for more than a few hours straight after everything is expelled.
-
If you think you did not expel everything from the uterus or if the placenta appears to be incomplete.
Something very important to consider is what to do with your baby after you deliver. I’m not talking about what to do while you’re waiting for burial, I’m talking about taking the baby with you to the doctor’s office or hospital. I strongly recommend that you do not do this. Call ahead to either location before you go (unless it is a genuine emergency, and even then it’s a good idea). If you are planning to take the baby with you, inform the staff that you will be bringing the baby but no one is permitted to touch him and he will remain in your custody. The reason is this: it has come to light that once the hospital takes possession, even for a moment, of your baby, they may refuse to give him back. They may insist on testing. There is no reason for them to do this unless you yourself wish to have testing performed. If you deliver in the hospital, you will automatically be up against this. [Note: I was informed by my doctor’s office after the fact that if anyone brings in the baby after having delivered at home, they are supposed to take the baby to the hospital pathology department. Somehow, they let me get away with bringing my baby in to show them and then returning home with him. Just a word of warning.]
Hospital disposal of babies varies with location but may include: cremation with medical waste before transport to a landfill, cremation with other babies with eventual burial (non-public location) and flushing into the sewer system. Babies under 20 weeks may be classified as medical waste or biohazard waste. This varies by state and by hospital. This is a hard truth, but it is better to know what you may be facing. People are working to change this.
[When I delivered my second lost baby, Andrew, I prepared a birth plan ahead of time that included everything I did and did not want done. I also discussed these things with my doctor before the date of induction. When I arrived at the hospital I gave the staff the birth plan (they made a copy and gave me the original) and discussed our wishes. We agreed on everything before the induction began. I am writing some specific suggestions concerning the birth plan and what I did at the hospital to ensure I would be able to take my baby home on a separate page.]
If you want to reassure the medical personnel, bring photographs (on your digital camera or phone) that you have taken of the baby. When I went to the doctor’s office for an exam and ultrasound the day after I delivered Innocent, I brought photographs of him. Not only were they able to see that I had indeed delivered a baby, but they were amazed at his beauty and detail. You can help change the medieval culture surrounding miscarriage.
===================================================
So what should I do?
Here is a list of the three management methods presented with pros and cons for each:
Expectant Management
Pros:
-
Lower risk to you: If you are generally healthy and do not have any complicating factors (such as a bleeding disorder or preexisting infection) then this represents the lowest risk way for you to miscarry. The risk of heavy bleeding is still present.
-
More privacy and ability to control your environment: This is also one of the reasons many women choose home birth over hospital birth. You are laboring and delivering, so this is not significantly different. This is an emotionally charged experience and many women do better with a friend or family member at their side (or within calling distance) in their own home than in the midst of bright lights and several strangers.
-
Psychological: You have been pregnant for a number of weeks, sometimes months, and you were doing all you could to provide a safe and nurturing environment for your child. Just because you are not facing the delivery of a live infant does not mean that you have stopped being a mother. Also, for some women, going through labor and delivery provides closure. Especially for a woman for whom this is a first pregnancy, going through the entire process from conception to delivery can reinforce the fact that she was really pregnant, that this is really a child, that she is really a mother.
Cons:
-
Psychological: If carrying a child for days or weeks after learning he has died is completely overwhelming (and in all honesty, it will not be easy), then a more rapid conclusion may be best. Whether this represents a D&C or pharmacological intervention, the physical miscarriage will be over and past in a few days (not counting recovery).
-
Risk of infection: If it is determined that the baby died several weeks ago, or you have already been waiting several weeks, and you haven’t had any physical signs of miscarriage, then you may be approaching the point at which a D&C is indicated. If you are already showing signs of infection (fever, foul-smelling vaginal discharge, abdominal pain), then you need medical intervention without waiting.
-
Heavy bleeding: There is a risk of heavy bleeding with this method especially if the placenta is not expelled.
Medical Management
Pros:
-
Psychological: You don’t have to endure as long a wait as you do with expectant management.
-
Privacy: If you are in the first trimester you will most likely be able to do this at home. (see above)
-
(same as expectant management)
-
[Note: if you have an ectopic pregnancy and are not in danger of rupture, this is the most likely way your medical practitioner will manage it. While some ectopic pregnancies do miscarry on their own, this is not the time for expectant management. Note that the medication is methotrexate rather than misoprostol.]
Cons:
-
Side effects of the medication include nausea, vomiting and diarrhea. It works by inducing uterine contractions so you will experience pain that may be more than if you had not taken the medication.
-
Hospitalization: If you are not in the first trimester (or even past 8 weeks, depending on your practitioner) you will probably be admitted to the hospital for the induction. If you are well into your second trimester expect to be admitted.
Surgical Management
Pros:
-
Quicker resolution: This is the most rapid resolution of a miscarriage. You could be scheduled as quickly as the next day for surgery.
-
Quicker recovery: You generally experience much less bleeding than with any other option, possibly less than a regular period.
-
[Note: if you have developed an infection or are bleeding heavily or have retained parts, this is not an optional procedure. Similarly, if you have an ectopic pregnancy that is in danger of rupture (or is rupturing) laparoscopy is not an optional procedure.]
Cons:
-
There are risks of infection, uterine perforation (a hole poked in your uterus) and uterine scarring that may make it more difficult to be pregnant in the future. The risk of scarring increases with additional D&Cs.
-
You will not have an intact body as a result. You will, however, still be able to request the remains for burial if you so desire.
*The most important thing is for you to have an honest conversation with your doctor or midwife about how you would like to manage your miscarriage, and to be willing to listen to her concerns about your health.
Many thanks to Dr. E. B. (ob/gyn) for contributions, suggestions and corrections!
===================================================
Natural Miscarriage Stories
1. Innocent’s birth story part II
[The larger story is in the “Your Stories” section. This is a more medical close-up. Innocent was born probably two and a half weeks after he died, one and a half weeks after we found out. This narrative is offered in the hopes that someone will have a better idea of what to expect.]
During the week before I learned we had lost Innocent at 12 ½ weeks I had noticed some of the more bothersome pregnancy symptoms easing. I had more energy, was less nauseated and was losing some of my food aversions. Oddly, and I couldn’t explain this, I was also losing the breast tenderness. I attributed everything to moving into the second trimester. Since this has been my experience with all of my other pregnancies, I was reassured that I was “right on track”. This kind of haunts me now that I know they all pointed to a fetal demise.
Fast forward to the second visit to the doctor when I had the ultrasound and set up the D&C for ‘just in case’. My cervix was long and closed. I was very discouraged because this seemed to indicate it would be a good while (if ever) before I started to miscarry naturally.
Two nights later, Saturday night, I noticed some brown spotting at 10:30. I was overjoyed. I wouldn’t be needing the D&C after all! By 11:30 the discharge was a little more red and I figured I’d be up for the rest of the night. Everything I had read suggested that it would be anywhere from several hours to a few days before the miscarriage was completed. I was cramping pretty hard now, almost to the point of contractions because they were coming in waves. I considered taking some pain medicine and trying to go to sleep thinking that I would almost certainly not sleep through the worst of it. Father was worried I would be too groggy if I did and unable to take care of myself. He doesn’t do well at all with blood so it was definitely going to be up to me. I had bought some super-massive overnight pads and some chux (disposable absorbent under pads) at the store the week before in preparation so I went ahead and put one on and tucked a chux under me. This was good thinking.
Not long after I felt a strange twisting ‘pop’ inside my lower abdomen. I wondered if something would happen. Nothing did. I picked up my book again. A few minutes later I felt something suddenly running out of me. I thought my water had broken but it turned out to be blood. Trying to think clearly I realized I had better go ahead and get to the bathroom because this was it. Father helped, and about ten minutes later I was in a tub of warm (not hot) water with supplies in easy reach. He left so he wouldn’t pass out but we left the door cracked so he could hear if I called. The tub was rapidly turning red and I had to manually remove a clot that felt glued to me. Not more than a minute later I felt a sensation of fullness and instinctively pushed. I felt something large come out. Even though I couldn’t see through the water I knew this was the baby. I was scared to reach down and feel around for it. I waited a minute, prayed for courage and after realizing that there was no one else to step in, reached down and gently picked up what turned out to be the amniotic sac with a large clot attached. I was unable to pick it up more than an inch above the water because I realized it was still connected to the umbilical cord. What a tiny cord! I thought that I would just support the sac until I delivered the placenta. Several minutes later it occurred to me that the placenta might be a good while coming. That’s when I realized I had forgotten something crucial: scissors. This was turning out to be closer to a regular delivery than I had expected. Father edged into the room to bring me a pair and I cut the cord.
I balanced a chux on my knees and put the sac on it. The fluid was cloudy, not clear, probably as a result of the extended time since the baby’s death. I was kind of scared to open it but I didn’t want to put the whole sac into the container of saline I had waiting. The baby was still floating around in the amniotic fluid and I suddenly saw very clearly a little foot and then a little white hand. I cut open the sac (it was surprisingly strong), the fluid flowed out and there he was. He was just beautiful. [photos on the “
photographs” page under 12 weeks] He was actually more developed than I had expected. He was somewhat pinkish-gray, very delicate and some of his skin had ‘blisters’ where fluid was collecting under it. This was from the physical processes of death. There were tiny shreds of skin, kind of like that you see on post-term babies, over most of his body, but they weren’t disfiguring. You mostly noticed these when he was in the saline later. After I held him for a minute and talked to him I put him in the saline and covered the container. Then I got down to the business of the rest of the delivery.
Over the next hour or so I passed about 10 clots of decent size. The water was so bloody that after about 45 minutes I let it out and refilled the tub. I still hadn’t delivered the placenta and I knew that I would keep bleeding until I did because the uterus was unable to fully contract to shut it down. There are a few options for assisting a placenta out but only one is possible when you are by yourself at home: fundal massage. I found the top of the fundus and pushed deeply into my abdomen, kneading it. After a minute or so of this (and I kept it up for a few minutes) I started having much stronger cramps. I passed another clot or two and then started trying bearing down. After a few pushes the placenta came out. I had to examine it to make sure it was all there and part not left inside. Now, placentas are not pretty. Frankly, they make me rather sick. Again, I realized that if I didn’t pick it up, no one else was going to (you don’t call the paramedics to pick up your placenta for you). I didn’t bother saving it for the doctor to look at because I was sure it was complete. I only passed one more medium-sized clot after that and blood, but the bleeding decreased significantly. I did a little more fundal massage to encourage the uterus to stay firm. All of the clots and the placenta I put in a chux and threw away. I recommend rinsing off with cool water, not warm, because the blood will come off better.
A few minutes after I got out of the tub and was cleaning up the bathroom I suddenly felt nauseated, hot and faint. I sat down but it got worse. I called to Father. I knew I was about to pass out and didn’t want to wind up on the floor. He helped me to bed (putting a chux down) and I lay there with my head down and my knees up and a cold washcloth on my face. I told him to get me something to drink. I checked my pulse to make sure I hadn’t lost too much blood but it was normal (otherwise it probably would have been high). I figured I just dropped my blood pressure from a combination of warm water, stress, pain and fluid loss. Fifteen minutes later I felt well enough to get up (slowly: sit with legs hanging down for a minute before standing), get dressed and finish cleaning up the bathroom. I made sure to finish the drink too. The last thing I did was spread out a clean chux and pick Innocent up out of the saline. I took pictures of him, taking full-body pictures of him in the saline and then in my hand and on the chux, then focusing on details like feet, hands, face, ears, etc. It also occurred to me to see if we could tell the sex. I wasn’t expecting to because of what I had read, but you could tell he was a boy. I put him back in the saline and wrapped the container before putting it in the refrigerator.
My bleeding that night was much less than what I had after full-term deliveries. It stayed bright red for almost a week and then rather quickly faded out. After a day it started up again in the middle of the night rather heavily and I passed a clot. Over the course of the next week it slowly turned from bright red to dark red, brownish red, brown, tan and now, just over two weeks later, it’s gone. [Update: I started a period four weeks from the date of delivery, two weeks after I stopped bleeding.]
2. Stephanie’s story of her natural miscarriage at 12 weeks.
This goes to show that not all miscarriages are alike but there are certainly many similarities. Stephanie is very specific and graphic (in a helpful way) in her description and so I am placing this story here as well as on the “Your Stories” page.
3. Amelia’s story of Micah’s birth at 15 weeks
Micah departed at the age of approximately 15 weeks. It was discovered a few weeks later and he was born after induction with misoprostol between 18 and 19 weeks. Unusually, Micah was born at home with the assistance of a midwife. Amelia does a very detailed job of describing the effects of a misoprostol-induced birth and gives a lot of helpful advice for anyone facing something similar.
4. Amber’s story of her miscarriage of a 7 week, 4 day baby at 11 weeks and 5 days
Amber’s story can be found on the “Your Stories” page. Amber had a missed miscarriage which was diagnosed 2 weeks after the baby’s death. She opted to wait for her body to deliver naturally and ultimately delivered her baby, “Our Angel Baby”, at home after 2 additional weeks.




















Shannen, I'm so sorry for your loss. Especially since you've been trying so long.
LikeLike
My friend going through a 5 months miscarriage home,she does want to go to the hospital. I want to know if she's safe to carry through I what I should do
LikeLike
My friend is going through a 5 months miscarriage at home,she doesn't want to go to the hospital because she was there for two weeks.. What are the procedures an necessary steps to take please help me out here
LikeLike
Kathy, your friend is essentially going to be attempting an unassisted home birth. I can't really give you medical advice and I don't know any of the circumstances or what her history is. I hope she called her doctor or midwife, or sought medical assistance in some way. A home stillbirth delivery is certainly possible, but it's impossible for me to know what the best decision for your friend would be. I'm very sorry for her loss.
LikeLike
This is similar to what I've experienced over the weekend. Reading your comment helped me feel normal as I've not read any other accounts that were relatable. Thank you for sharing.
LikeLike
I am currently waiting to naturally miscarry.. Diagnosed blighted ovum at 7 weeks 2 days and then confirmed at o weeks 2 days. I think things are starting. I'm having waves of some pretty intense cramps and have had some spotting today. I am emotional right now even though I have been preparing myself for weeks. The worst thing I have had people say is “at least there isn't really a baby”. This was my pregnancy, this was my baby. My baby died sooner than others but it was still my baby. I loved my baby. I looked forward to my baby. I had dreams and thoughts and hopes for my baby..
LikeLike
Yes, there “really is a baby.” People are sadly misinformed on the matter. I'm so sorry for your loss. I hope your body reaches a resolution soon and that you are able to find peace. I've never heard from anyone who regretted waiting to miscarry naturally (although for medical reasons it is not always possible). That in and of itself is a factor in healthy grieving. ((Hugs))
LikeLike
I thought I was over my natural miscarriage and then the next day I started getting intense contractions and more clots. Luckily all my kids were occupied at the time. I went to the bathroom and looked down and saw a big clot that was kind of stuck so I beared down and pushed a 3″ by 1.5″ wide clot out. I was for sure it was the baby. I came to your site and saw the pic that looked just like what I had pushed out. I broke it open but only saw placenta. I never saw a clear sack or a baby. The baby had passed at 6weeks 3 days and I pushed it out at 9 weeks 6 days. Do you think the baby was in one of the many clots I had passed during a very intense four hours the day before? I went through the last clot very finely and didn't see anything.
LikeLike
Desi, I'm very sorry for your loss. It's difficult to say for sure from this vantage point, but if you did not see a sac that last time then yes, it's possible you already passed it. Alternatively, given the amount of time that has passed, the sac may have not been intact. In that case it would be nearly impossible to find.
LikeLike
Thank you so much to all of the brave women who have posted on this site. This is the single most helpful resource I have seen about miscarriage online, hands down. There are so many clinical websites that explain symptoms, but hardly anywhere can you actually read what it actually *feels* like and *looks* like, and as I am going through this myself, reading other people's experiences has been reassuring, comforting, and unbelievably helpful. So thank you.
I was diagnosed with an empty sac pregnancy last week, and following one week of spotting — first brown, then red — this morning I finally started to bleed heavily (slightly heavier than a period). It felt like I was having period cramps. On the toilet I passed what I'm assuming was the sac into the toilet paper – it was white/gray tissue that looked a bit like wrinkled gelatin. I had been reading posts about passing the sac, and I'd already passed a lot of clots assuming I'd missed the sac somehow. I can now say from experience that you will *know* IF and when you see it because it is different from everything else coming out of you.
I thought, ok finally this is it…. But then the bad cramping started. After a couple of hours it was clear that they were contractions, as they had a clear start and stop. I was fine in between them; then they'd pick up again, etc. Advil didn't do much of anything. Eventually, these cramps/contractions became excruciating, and the period of relief in between that I'd had earlier in the day diminished. At their worst, the only place I felt comfortable was on the toilet, even though I didn't have to use the bathroom. All of a sudden I had a big and uncontrollable gush of blood into the toilet, and then there seemed to be something in my vagina – before I knew what was happening, my body just pushed naturally. And out came something solid, about the size of a golf ball. My pain immediately stopped, and I stood up, in shock. With my husband at my side we picked up what I had expelled in the toilet. From reading this post it very much seems that this was the placenta, which came about five hours after I'd (nearly) painlessly expelled the sac. I had read *nowhere* that with a blighted ovum (empty sac pregnancy) there would also be an afterbirth, and possibly at a different time.
It was frightening to pass the sac in the morning, then thinking I was through it (finally), only then to have the pain and bleeding increase. If anyone is worried about this, it could be you have yet to pass the placenta. I had about 4 hours in between each passage. I'm still bleeding in the hours after, but I can already tell it is starting to subside slightly. Though we had no physical baby, the emotional pain is real, and we mourned the passage of the tissue my body had been growing for these last 7 weeks. I hope it helps to share my own story — you have all been such a comfort and help to me. Sending my thoughts and prayers to you all.
LikeLike
Elizabeth, I'm very sorry for your loss. Thank you for sharing your story.
LikeLike
So is it possible for the sac and placenta to pass all at once? I had labor like contractions for 2.5 hours. I passed some clots but they were not big at all. Just little ones and maybe the biggest was the size of a penny. I was sitting on the toliet and suddenly something larger and unmistakable just fell out. It looked like a ball of tissue with the raw hamburger like placenta attached (ugh) The contractions and pain completely went away as soon as that happened. Do you think my miscarriage completed at that point? I have no health insurance and the tests the doctors want to do are very expensive and the last thing we need right now are more bills. I know that sounds bad but I'm just unsure what to do. The doctor said if I don't want to go in to just monitor the bleeding. She said as long as my blood type is positive, no irregular bleeding occurs, and I show no signs of fever or infection I should be in the clear. Thoughts? Also thank you for the information on this website. It has been helpful.
LikeLike
Anonymous, yes, your doctor was right. And yes, you can pass everything at once, especially earlier in pregnancy. I'm sure you completed the miscarriage at that point because you noticed the bleeding and cramping lessened immediately. As long as you're not bleeding such that you're saturating a pad an hour, running a fever, having foul-smelling drainage, have pain that does not go away or is getting worse, passing out, or nausea and vomiting, you are fine to rest at home until your follow up appointment. Stay hydrated and rest.
I'm so sorry for your loss.
LikeLike
I just passed my babies at home through natural miscarriage, and as I'm sitting here, I am aware that the cramps & physical pain is gone, that my body feels an incredible peace, and my soul feels incredibly one-on-one with nature & probably God right now. I went through this myself today, although I called the babies' father as well as my sister, letting them know the process began and that I was afraid. I feel that there is not much else that could happen to cause this type of sadness. I have been writing to my babies since the day before I officially received the doctor's word that yes, I was pregnant. And then I went in for the first sonogram, only to hear no heartbeat. I had to wait over a week to get a transvaginal ultrasound, at which i could clearly see two babies, one with a rapid heartbeat, the other none. Not that it's a focus right now, but at that ultrasound, a number of fibroids and large cysts were also found, of which i'll eventually face at my next appointment. At the follow-up ultrasound the following week, the silent/sad technician and the 'non-movement' on the screen revealed that my other baby did not make it. They were Thomas & Iris, to me. The day I learned of first baby's passing, was also the day my step-father-figure passed, and it was on the day of his burial that I learned of my second baby's passing. I don't want to be around others at the moment. I want to be right where I am, listening to the birds, not wanting nightfall to come, writing to whomever may read this, and thinking on how much I miss the lives I won't be sharing. I feel stronger & sadder that I have ever in my life. I was so ready to finally be a mom. I love them, and I will do good things in their honor.
LikeLike
May their memory be eternal!
LikeLike